
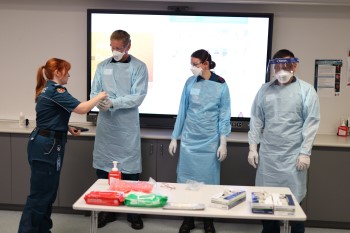
A simple but effective visual exercise conducted during a graduate paramedic induction session at Whyte Island recently served as an excellent reminder of the importance of infection control in everyday Queensland Ambulance Service (QAS) responses.
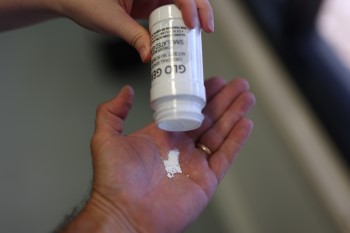
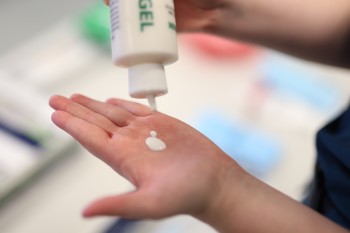
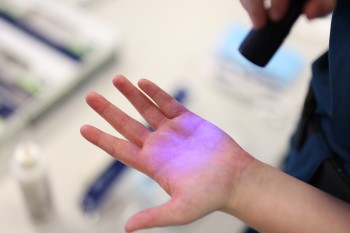
While Infection Prevention and Control’s Acting Statewide Infection Prevention Program Coordinator Jemma Shirra-Gibb had used this exercise to demonstrate how easily invisible germs can spread, it also highlights why this role is vital to our service.
“In a nutshell, our responsibility is to help mitigate any infection-related risks to our people and patients, and to ensure our service can continue to deliver safe, high-quality care to our community,” Jemma said.
“Healthcare acquired infections actually account for the highest number of complications sustained whilst in the care of a health service in Australia.
“If we practice sub-optimal infection control, we risk patients having to re-present to our service and take up beds in hospitals.
“There was recently a study in Scotland that showed infections acquired as a complication of healthcare actually accounted for patients spending, on average, seven days longer in their length of hospital stay.
“As we all experienced with the COVID-19 pandemic, exposure to infectious diseases can have severe consequences for our staff, both in terms of our own health, and the potential to spread illness to our families.
“Infection Control is imperative to patient safety, as these people are often already in a vulnerable state, and the last thing they need is to acquire an additional bug on top of that.
“Some of our more vulnerable cohorts may not have the energy to fight an infection on top of their primary reason for calling us to attend a hospital.”





Infection control is central to maintaining operational continuity.
“If staff become ill in groups, it can significantly impact the QAS’s ability to respond and provide care to our communities – a healthy workforce is crucial to maintaining this continuity of care, and we don’t want our staff bringing home any nasty bugs to their families,” she said.
“We also have to remember we have an ethical obligation to protect both staff and patients from preventable harm.”
The Infection Control team has several key responsibilities which combined, provide a multifaceted approach through education, risk management and systemic improvements to protect staff and patients from the spread of infectious disease. These include;
- Staff safety and exposure management
- Contact tracing
- Education and training
- Staff health systems
- Quality Improvement projects
- Antimicrobial stewardship
- Product review and testing
- Policy and procedure integration and optimisation
- Collaboration and preparedness
- Monitoring epidemiological trends, both locally and globally
- Mentoring officers around the regions who’d like to upskill in the area
“On a day to day basis, the work we do is constantly changing, is quite varied, and we focus heavily on ensuring our workforce’s safety - probably about 60 per cent of the time,” Jemma said.
“No day is the same and I never know what to expect walking in the door.”
“This will include raising awareness of outbreaks to protect our staff, from exposure to infectious diseases like measles, meningococcal and tuberculosis, all of which we are seeing a resurgence of globally.
“We’re responsible for contact tracing when staff are exposed to any infectious diseases, and we will conduct investigations to identify exposed staff and link them in with accessing any necessary post-exposure prophylaxis if needed, so they can return home safely to their families,” she said.
“The team delivers regular educational workshops and staff training covering topics like infection control practices, proper PPE use and identifying signs of infectious diseases.
“Last year, we revamped the GPIP Infection Control workshop to be more interactive and have had great feedback so far, especially with our use of UV powder to enable our graduates to visualise how far those germs can go.”
Jemma said the team has a role in reviewing and testing new products and equipment to ensure they meet infection control standards and are appropriate for use in the field.
“We are currently working to integrate infection control considerations into existing policies, procedures and resources to make them more user-friendly and effective for frontline staff.”
Jemma said the recent experiences from COVID-19 highlighted the need to plan for the next potential “Disease X” pandemic, but we would need to remain vigilant with ongoing monitoring and preparedness which can be difficult to maintain long-term.
Looking ahead: Don’t become an April Flu-ul
Jemma is calling on staff to embrace our annual influenza vaccinations and make use of the free vaccinations provided to all staff.
“We’re 4-8 months behind the northern hemisphere’s trends and it’s looking like we are in for a severe flu season this year,” she said.
“America has recorded its first ‘high severity’ flu season since 2017, meaning the country is experiencing higher than normal hospitalisations, deaths, and use of outpatients (i.e., GP) appointments.”
Jemma said the best time to have your flu vaccination in Australia was between April and June.
“QAS immunisation clinics are happening again throughout the regions,” she said.
We also have linked with the Pharmacy Guild to organise free flu vax bookings if you cannot access via QAS clinics: dates/codes qldambulance.sharepoint.com/sites/intranet/clinical/influenzastrategy/Pages/default.aspx
“We would recommend staff aged 65 and older, or who are pregnant, or immunocompromised can access a more effective vaccination via GPs/pharmacies, rather than being immunised through the QAS immunisation clinics.”